An important paper has been published in the journal Clinical Oncology. This meta-analysis, entitled “The Contribution of Cytotoxic Chemotherapy to 5-year Survival in Adult Malignancies” set out to accurately quantify and assess the actual benefit conferred by chemotherapy in the treatment of adults with the commonest types of cancer. Although the paper has attracted some attention in Australia, the native country of the paper’s authors, it has been greeted with complete silence on this side of the world.
All three of the paper’s authors are oncologists. Lead author Associate Professor Graeme Morgan is a radiation oncologist at Royal North Shore Hospital in Sydney; Professor Robyn Ward is a medical oncologist at University of New South Wales/St. Vincent’s Hospital. The third author, Dr. Michael Barton, is a radiation oncologist and a member of the Collaboration for Cancer Outcomes Research and Evaluation, Liverpool Health Service, Sydney. Prof. Ward is also a member of the Therapeutic Goods Authority of the Australian Federal Department of Health and Aging, the official body that advises the Australian government on the suitability and efficacy of drugs to be listed on the national Pharmaceutical Benefits Schedule (PBS) – roughly the equivalent of the US Food and Drug Administration.
Their meticulous study was based on an analysis of the results of all the randomized, controlled clinical trials (RCTs) performed in Australia and the US that reported a statistically significant increase in 5-year survival due to the use of chemotherapy in adult malignancies. Survival data were drawn from the Australian cancer registries and the US National Cancer Institute’s Surveillance Epidemiology and End Results (SEER) registry spanning the period January 1990 until January 2004.
Wherever data were uncertain, the authors deliberately erred on the side of over-estimating the benefit of chemotherapy. Even so, the study concluded that overall, chemotherapy contributes just over 2 percent to improved survival in cancer patients.
Yet despite the mounting evidence of chemotherapy’s lack of effectiveness in prolonging survival, oncologists continue to present chemotherapy as a rational and promising approach to cancer treatment.
“Some practitioners still remain optimistic that cytotoxic chemotherapy will significantly improve cancer survival,” the authors wrote in their introduction. “However, despite the use of new and expensive single and combination drugs to improve response rates…there has been little impact from the use of newer regimens” (Morgan 2005).
The Australian authors continued: “…in lung cancer, the median survival has increased by only 2 months [during the past 20 years, ed.] and an overall survival benefit of less than 5 percent has been achieved in the adjuvant treatment of breast, colon and head and neck cancers.”
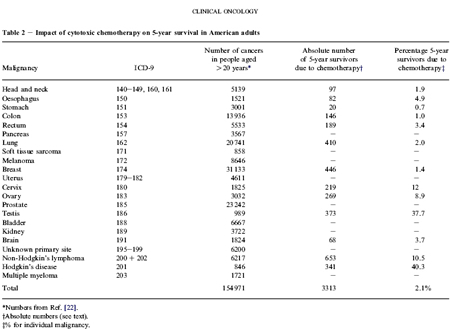
The results of the study are summarized in two tables, reproduced below. Table 1 shows the results for Australian patients; Table 2 shows the results for US patients. The authors point out that the similarity of the figures for Australia and the US make it very likely that the recorded benefit of 2.5 percent or less would be mirrored in other developed countries also.
(NB: We apologize for the poor image quality of these tables. The blanks in the columns represent zero, i.e. no direct benefit can be attributed to chemotherapy; no patients in that category achieved an increased 5-year survival due to chemotherapy.)
Table 1
Results for Australian patients
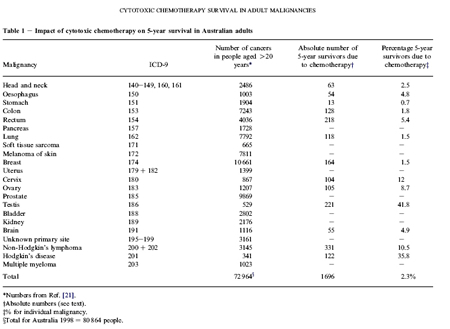
larger image
source: http://www.cancerdecisions.com
Table 2
Results for US patients
larger image
source: http://www.cancerdecisions.com
Basically, the authors found that the contribution of chemotherapy to 5-year survival in adults was 2.3 percent in Australia, and 2.1 percent in the USA. They emphasize that, for reasons explained in detail in the study, these figures “should be regarded as the upper limit of effectiveness” (i.e., they are an optimistic rather than a pessimistic estimate).
Understanding Relative Risk
How is it possible that patients are routinely offered chemotherapy when the benefits to be gained by such an approach are generally so small? In their discussion, the authors address this crucial question and cite the tendency on the part of the medical profession to present the benefits of chemotherapy in statistical terms that, while technically accurate, are seldom clearly understood by patients.
For example, oncologists frequently express the benefits of chemotherapy in terms of what is called “relative risk” rather than giving a straight assessment of the likely impact on overall survival. Relative risk is a statistical means of expressing the benefit of receiving a medical intervention in a way that, while technically accurate, has the effect of making the intervention look considerably more beneficial than it truly is. If receiving a treatment causes a patient’s risk to drop from 4 percent to 2 percent, this can be expressed as a decrease in relative risk of 50 percent. On face value that sounds good. But another, equally valid way of expressing this is to say that it offers a 2 percent reduction in absolute risk, which is less likely to convince patients to take the treatment.
It is not only patients who are misled by the overuse of relative risk in reporting the results of medical interventions. Several studies have shown that physicians are also frequently beguiled by this kind of statistical sleight of hand. According to one such study, published in the British Medical Journal, physicians’ views of the effectiveness of drugs, and their decision to prescribe such drugs, was significantly influenced by the way in which clinical trials of these drugs were reported. When results were expressed as a relative risk reduction, physicians believed the drugs were more effective and were strongly more inclined to prescribe than they were when the identical results were expressed as an absolute risk reduction (Bucher 1994).
Another study, published in the Journal of Clinical Oncology, demonstrated that the way in which survival benefits are presented specifically influenced the decision of medical professionals to recommend chemotherapy. Since 80 percent of patients chose what their oncologist recommends, the way in which the oncologist perceives and conveys the benefits of treatment is of vital importance. This study showed that when physicians are given relative risk reduction figures for a chemotherapy regimen, they are more likely to recommend it to their patients than when they are given the mathematically identical information expressed as an absolute risk reduction (Chao 2003).
The way that medical information is reported in the professional literature therefore clearly has an important influence on the treatment recommendations oncologists make. A drug that can be said, for example, to reduce cancer recurrence by 50 percent, is likely to get the attention and respect of oncologists and patients alike, even though the absolute risk may only be a small one – perhaps only 2 or 3 percent – and the reduction in absolute risk commensurately small.
To their credit, the Australian authors of the study on the effectiveness of chemotherapy address the issue of relative versus absolute risk. They suggest that the apparent gulf between the public perception of chemotherapy’s effectiveness and its actual mediocre track record can largely be attributed to the tendency of both the media and the medical profession to express efficacy in terms of relative rather than absolute risk .
“The minimal impact on survival in the more common cancers conflicts with the perceptions of many patients who feel they are receiving a treatment that will significantly enhance their chances of cure,” the authors wrote. “In part this represents the presentation of data as a reduction in risk rather than as an absolute survival benefit and by exaggerating the response rates by including ‘stable disease.'”
As an example of how chemotherapy is oversold, they cite the treatment of breast cancer. In 1998 in Australia, out of the total of 10,661 women who were newly diagnosed with breast cancer, 4,638 women were considered eligible for chemotherapy. Of these 4,638 women, only 164 (3.5 percent) actually gained some survival benefit from chemotherapy. As the authors point out, the use of newer chemotherapy regimens including the taxanes and anthracyclines for breast cancer may raise survival by an estimated additional one percent – but this is achieved at the expense of an increased risk of cardiac toxicity and nerve damage.
“There is also no convincing evidence,” they write, “that using regimens with newer and more expensive drugs is any more beneficial than the regimens used in the 1970s.” They add that two systematic reviews of the evidence been not been able to demonstrate any survival benefit for chemotherapy in recurrent or metastatic breast cancer.
Another factor clouding the issue is the growing trend for clinical trials to use what are called ‘surrogate end points,’ as a yardstick by which to measure a chemotherapy regimen’s effectiveness. This is instead of using the only real measures that matters to patients – prolongation of life as measured by overall survival and improved quality of life. Surrogate end points such as ‘progression-free survival,’ ‘disease-free survival’ or ‘recurrence-free survival’ may only reflect temporary lulls in the progression of the disease. Such temporary stabilization of disease, if it occurs at all, seldom lasts for more than a few months at best. The cancer typically returns, sometimes with renewed vigor, and survival is not generally extended by such interventions. However, trials reported in terms of surrogate end points can create the illusion that the lives of desperately ill patients are being significantly extended or made more bearable by chemotherapy, when in reality this is not the case.
In summary, the authors state:
“The introduction of cytotoxic chemotherapy for solid tumors and the establishment of the sub-specialty of medical oncology have been accepted as an advance in cancer management. However, despite the early claims of chemotherapy as the panacea for curing all cancers, the impact of cytotoxic chemotherapy is limited to small subgroups of patients and mostly occurs in the less common malignancies.”
Splitting Hairs
In view of the highly controversial nature of the study’s findings, one might have expected it to receive enormous international attention. Instead, media reaction has been largely limited to the authors’ native land of Australia; the study received almost no coverage whatsoever in the US. In fact, although the paper appeared in December 2004, there was limited coverage even Down Under. The authors were interviewed for the Australian Broadcasting Corporation (ABC) program The Health Report in April 2005. But their landmark paper did not come to most doctors’ attention until a widely distributed medical practice periodical, the Australian Prescriber, ran an editorial on the study early in 2006.
On ABC’s The Health Report, Prof. Morgan, the paper’s principal author, reiterated the study’s conclusions that chemotherapy had been oversold, and pointed to the fact that relative risk reduction is being used as the yardstick of efficacy, with its deceptively large percentage differences.
For balance, the show host, Norman Swan, interviewed Prof. Michael Boyer, chief of medical oncology at Australia’s Royal Prince Albert Hospital, Sydney. Unable to deny the validity of the study’s essential findings, Prof. Boyer instead attempted to nitpick the authors’ methodology. He suggested that the figure for chemotherapy’s efficacy was actually somewhat higher than the study had concluded. Yet even so, when pushed, the most favorable figure he could come up with was that chemotherapy might actually be effective in 5 or 6 percent of cases (instead of around 2 percent).
Interviewed by Australian Prescriber, Prof. Boyer similarly commented: “If you start…saying how much does chemotherapy add in the people that you might actually use it [in], the numbers start creeping up…to 5 percent or 6 percent” (Segelov 2006).
In my opinion, this sort of hair-splitting damns chemotherapy with faint praise. It actually confirms the central message of the three critics’ study. If the best defense of chemotherapy that orthodox oncology can come up with is that it may actually be effective for 5 or 6 percent of cancer patients, rather than merely 2 percent, then surely it is high time for a radical reassessment of the widespread use of this toxic modality in cancer treatment. Either figure – 2 percent or 6 percent – will come as a shock to most patients offered this type of treatment, and ought to generate serious doubt in the minds of oncologists as to the ethics of offering chemotherapy without explicitly warning patients of its unlikely prospects for success.
It was also astonishing that the orthodox Prof. Boyer complained that one of the major shortcomings of the study was that it insisted on measuring absolute instead of relative benefits. Asked by the interviewer whether there weren’t violations of informed consent implicit in the way that benefits of treatment were usually presented, Prof. Boyer defended the use of the more impressive-sounding relative risk reduction:
“One of the problems of this [Morgan, ed.] paper is it uses absolute benefits rather than relative benefits,” he protested: “…the relative benefit is about a one third reduction in your risk of death.”
This, of course, is precisely the reverse of the argument made by the study’s authors, who clearly demonstrated the misleading nature of relative risk reduction as a means of describing the efficacy of chemotherapy.
Other Critics Emerge
Prof. Morgan and his Australian colleagues are not alone in criticizing the pervasive use of relative risk as a means of inflating treatment efficacy. There have been others in recent years who have also voiced concern about this trend. For example, in a letter to the editor of the medical practice journal American Family Physician, James McCormack, PharmD, a member of the faculty of Pharmaceutical Sciences, University of British Columbia, made this same point about relative vs. absolute risk with great clarity.
Dr. McCormack took as an example the prescription of the bisphosphonate drugs in the treatment and prevention of osteoporosis…but identical issues apply to the use of anticancer drugs. The journal in question had written that one of those drugs produced almost “a 50 percent decrease” in the risk of new fractures. Addressing himself to a hypothetical patient, Dr. McCormack reinterpreted this statement in terms of absolute risk: “Mrs. Jones, your risk of developing a…fracture over the next three years is approximately 8 percent. If you take a drug daily for the next three years, that risk can be reduced from 8 percent to around 5 percent, or a difference of just over 3 percent.” Of course that sounds far less impressive than saying that taking the drug will decrease the risk of fracture by almost half, even though technically both are mathematically accurate ways of expressing the benefit to be gained by the therapy.
The Good News and the Bad
News concerning conventional cancer treatments seems to come in two varieties: good and bad. Good news, meaning that conventional treatments work well, often generates widespread press coverage and enthusiastic statements from health officials. On the other hand, bad news, such as the fact that conventional treatments have generally been oversold, usually comes and goes unseen, attracting no media attention whatsoever.
An example of the first kind is the recent announcement that for the first time in 70 years, the absolute number of US cancer deaths had fallen. Andrew C. von Eschenbach, MD, director of the US National Cancer Institute (NCI), called this “momentous news.” Similarly, Dr. Michael Thun, head of epidemiological research for the American Cancer Society, said it was “a notable milestone.” How big was the celebrated decline? As we reported in a recent newsletter, deaths actually fell by a total of 370, from 557,272 in 2003 to 556,902 in 2004. Expressed as a percentage of the total, it represents a drop of seven hundredths of one percent (0.066 percent).
Contrast the wildly enthusiastic coverage given to this tiny improvement in the annual cancer death rate with the almost total media blackout (at least in North America) on this critical paper from Australia. Yet nothing can obscure the fact that chemotherapy, for most indications, has far less effectiveness than the public is being led to believe. Dr. Morgan and his colleagues deserve every reader’s gratitude for having pointed this out to their colleagues around the world.